New Treatments For Interstitial Cystitis, UTI And Prostatitis
Article by:
New treatments for Interstitial Cystitis (IC) are often discussed and sometimes pursued within the medical community. In the UTI patient community, conversations about a bacterial component for IC patients are common.
In this video, Dr. Tim Hlavinka lays out the advantages of using DNA testing methods to identify organisms and guide new treatments for Interstitial Cystitis patients.
Dr. Hlavinka also touches on the impact of foreign materials, or implants, in the body and the differences between his prostatitis and UTI treatment approaches.
Watch the video or read the full transcript below to learn more.
Jump To Section:
- Video 4 Transcript: New Treatments For Interstitial Cystitis >>>>
- Bacterial Involvement for Interstitial Cystitis Patients >>>>
- What About Other Treatments for Interstitial Cystitis and UTI? >>>>
- Determining Success of Interstitial Cystitis Treatments >>>>
- Do People With Recurrent UTI Actually Recover? >>>>
- How do Implants in the Body Contribute to UTI? >>>>
Video 4 Transcript: New Treatments For Interstitial Cystitis, UTI And Prostatitis
Melissa: So I wanted to ask you a couple of questions about recurrent UTI and IC treatment and how you work with your patients. The first question is, do you have any general advice for people whose symptoms disappear when they take antibiotics and then return again a short time later?
Dr. Hlavinka: IC is changing, the field around IC is changing. I believe the thought leaders in Interstitial Cystitis and urology and urogynecology and women’s health have taken on the notion that we have a large component of Interstitial Cystitis which is undiagnosed or under-diagnosed infection.
In my own practice that was one of the first subset of patients that I discovered the benefits of next generation sequencing technology, because the patients acted as if they had an infection on top of their Interstitial Cystitis. They complained of worsening symptoms when they had a urinary tract infection and knew exactly what those symptoms were like. But then the failure of the traditional cultures to be able to deliver results that we could use to treat successfully was a big part of that.
So, those were among the most helpful. I think at least a half a dozen of them at the very beginning which sold me quickly on next generation sequencing particularly in patients for whom infection symptoms on top of another entity could be problematic.
Why Next-Generation Sequencing Can be Helpful When Other Conditions are Present
Dr. Hlavinka: So, I would say, and I’m getting stronger by the day from the standpoint of my emphasis on this, and that is, if you have an infection or history of infections and you think you have an infection or if you have a chronic condition which is exacerbated by an infection on top of it, complicating it, then I would demand your doctor learn how to do next generation sequencing and run that test.
Because you will find, in my case, probably 80-90% of the patients, indeed I was interviewed last week by a lab asking for clinical relevance. I told them that we really have to rethink what we call an infection these days, and limitations in technology are the most important thing.
Bacterial Involvement Guiding Treatment for Interstitial Cystitis Patients
Melissa: You mentioned people that have been diagnosed with IC that have an infection on top of their IC, which is the language that we hear a lot. If they have been culturing negative and then sometimes they culture positive, which is when they say they have the infection, do you think the whole set of their symptoms could actually be caused by infection, or that they do have a UTI on top of whatever else is happening?
Dr. Hlavinka: I think the simplest thing to do is to identify and treat, and if you identify with next generation sequencing you’ve done everything you can. Now some of those are frustrating in that even then the NGS is negative. However, I just took a lady to the operating room last week and we were going to do biopsies of her lesions because we’d talked about that. It turned out that she actually had an ulcer and the ulcer was positive and we sent that for tissue analysis and that showed the infection.
Biopsies from Interstitial Cystitis Patients Reveal Bacteria
Dr. Hlavinka: So I’m convinced that IC is probably either bacteria or bacterial product buried under the surface much like acne is or much like cellulitis is where you really don’t have the infection on the surface. There’s not an abscess or a pustule or something like that, that’s a medical term, but you know, a big round pocket of infection like a pimple.
A pustule is a pimple, the classic white head. So you see these in the bladder on endoscopy and you say well that’s got to be something, that’s got to be infection, so my goal is to biopsy as many as I can.
Now, good news, bad news – the bad news is I’m not finding them, and the good news is that because I’m doing the MicroGenDX ahead of time, finding them and treating them, the findings on endoscopy are less pronounced.
I’m still seeing the occasional pimply bladder as I call it and I’m going to start biopsying those and sending them. And dollars to dimes, or pounds to pence, is that what you say there? Pounds to pence, it’s going to be an infection.
How Other Conditions Impact Recurrent UTI Treatment
Melissa: If you do find infection in an IC patient, is the treatment the same as you would use for a recurrent UTI patient?
Dr. Hlavinka: I had a brilliant urogynecologist talk about female pelvic floor issues. And the notion of physiologic pelvic floor dysfunction, like from prolapse or hypertonicity, was one corner of the diamond. The other was pure IC. The other was pure infection and the other was pure overactive bladder, neurological bladder.
You form this diamond, can you see that? At the corners were these, and his point was that every woman is somewhere in there, who’s had these conditions before. They’re not pure pelvic floor, pure IC.
So if you think of this as sort of a constellation of entities that contributes one versus the other and sure the pelvic floor may manifest if you’re had ten infections in a row and your IC is flaring and your overactive bladder, and you’ve had a rough week with diet or something. So I tend to think of it this way.
Every time I see a woman who is flaring, whatever her diagnosis, that means even if she comes in as pure overactive bladder, I do the same thing – could this be the other three? By not treating all four of those at once, you’re really not getting the patient to improve as fast as you possibly can.
When I said that it means I’ve probably got to do that. She’s probably going to get a boost in her overactive bladder medication, maybe Interstitial Cystitis therapy enhancement, maybe a referral back to a physical therapist or whatever helped her in the past, so that’s how I would approach that.
It would be great to say that they all got better just with antibiotics, but I can’t say that.
Long-Term Antibiotics as a Recurrent UTI Treatment
Melissa: What’s your opinion on long term, full-dose antibiotics, like the protocol that is often used in the UK?
Dr. Hlavinka: I am changing. I was a big fan of suppressive antibiotics in the past. Many times that was all we had. The problem is, if you’re dealing with inadequate information or misinformation or negative cultures or inaccurate cultures and you put somebody on long term antibiotics, you’re basically calling this a therapeutic end point and you’re saying I’m going to be satisfied with clinical outcomes. And obviously that’s ok, if it’s ok. And that’s not glib.
The bottom line is that many times doctors say ‘you’re ok’, I’ve got you on the right antibiotic, the culture says you’re on the right antibiotic, 90 days, see you… And you’re not good, you’re not happy and you’re coming and telling me that your symptoms are worse. So my experience with the refractory recurrent urinary tract infection patients is that they weren’t doing well, and either I gave up because I didn’t have anything else to offer or I had to ask them to live with their symptoms.
And we kept jumping ahead, staying one ahead with the next antibiotic. I would say that’s ok, as long as you use the latest technology to identify what organisms are there. Next generation sequencing is better at identifying, but it doesn’t do anything bacterial resistance because micro-organisms are smart and they don’t like being found out. They like to get away with therapeutic madness.
So my opinion is that it would be ideal to use a combination of prevention, a combination of shorter interventions, a combination of antimicrobials that aren’t antibiotics and sort of an overall program of health that is better than that. Now, if you get to the point where you’ve tried all that and there’s nothing else but a daily, single antibiotic, sure, I still do that.
What About Other Treatments for Interstitial Cystitis and UTI?
Melissa: What about bladder instillations, do you ever recommend those for your patients? Antibiotic bladder instillations that is.
Dr. Hlavinka? In most of the ones that I’ve had to do are patients with complicated urinary tract infections from either neurologically mediated issues, retention due to spinal cord injury, multiple sclerosis, stroke, things like that, or they have chronic indwelling catheters or something – some complicated urinary tract history where I really don’t have any choice.
I haven’t had that many patients benefit from bladder instillations and the invasiveness of it, in order to put a catheter in, once or twice a week, and instil the bladder. Typically I will add antibiotics in a patient with an IC flare, I’ve found that helps.
I also add antibiotics to my botox injections for the patients with overactive bladder because I feel the particular aminoglycoside antibiotic, I think it helps prolong the benefit of the botox. But the instillations in patients that can feel and have to catheterize themselves, they’re uncomfortable and are also a chance for infection if not done correctly.
What About Bladder Fulguration?
Melissa: What about bladder fulguration, do you ever use that technique and can you briefly explain what it is?
Dr. Hlavinka: Do I look that old, Melissa? I mean, just kidding. So the older urologists, and there may be a place for that. There are – everything that’s old is new again – and the newer fulguration of the pseudo membranous cystitis and the acne of the bladder that I called earlier the ‘cystitis cystica’, the fulguration of that, I can see that that can be beneficial. I don’t do it.
Again I feel like the tools are just not there to define that. We just don’t really know what that is and scarring can happen at any time. It can happen the first time. I’ve had a patient get a urethral stricture, a female which is rare, get a urethral stricture from a single catheterization during an epidural, during her delivery.
And so the bladder mucosa, the bladder lining is a very delicate thing, especially in someone who has had recurrent infections, or IC and all these other irritative issues. Why nuclear them with thermal energy or laser energy? I don’t see it.


Healthy vs damaged bladder lining
Diagnosing and Treating Recurrent UTI
Melissa: So, what is your general approach to diagnosing and treating recurrent UTI?
Dr. Hlavinka: Again, when you have a referral practice like mine, you already have gotten 5-15 negative cultures or useless cultures, or cultures that showed something, but it was not the right thing to treat, so why waste my time with something like that?
Sure, in the rare case where I get a next generation sequencing naive patient, yeah I’ll probably go through some traditional cultures or a PCR (polymerase chain reaction) is sort of in between traditional cultures and next generation sequencing. But that’s just so rare these days that it’s probably one in a hundred patients. I go straight to next generation sequencing, I look at the organisms that are shown in the distribution.
I’m very specific about how the specimen is delivered because if they’ve just finished antibiotics or are still on antibiotics it’s useless. In fact four days is probably about the minimum to be able to get any meaningful information. And then once I see the organisms I decide which way to treat.
I try to do, because this is new information most of the time, and by the way, the question was asked during a presentation last week – how many are negative at the outset? How many are negative or not helpful, with a contaminant or something. And that number in our now database of over 800, is 8%.
Of those, if I kind of threw out the ones that were too soon, I bet the number is even lower. So that’s a big number of goodness in your initial diagnosis.
Determining Success of New Treatments for Interstitial Cystitis
Dr. Hlavinka: Now does that mean I took 92% of patients with recurrent UTIs, I did their first next generation sequencing and I cured them in ten days of antibiotics?
Well, no, because again this is a really tough disease with all sorts of multiple contributing factors and so under those circumstances that’s what I start with. I treat it. I try to do a shorter course because I just want to see what treating the correct organism does and then we observe.
Again, the whole notion of what is an eradication of an infection these days is changing because a negative culture means nothing to me. And I can’t tell you that getting rid of the organism on the next generation sequencing is the goal either because often that’s elusive. You can get a decrease in the reads, which is just sort of the copies of the DNA the machine reads.
So I use decrease in reads. If I don’t get any decrease in reads, even if it was sensitive by the recommendations of the panel, I think that’s a failure. If a patient had no symptoms and I didn’t decrease the reads at all on the next generation sequencing, would I consider myself a success? No, that’s not enough. I think that the next generation sequencing is so precise that it’s really not appropriate to say that we’ve done anything without that.
So that’s kind of how I do it and then we just observe and we repeat and we treat and we try these other things that we’ve talked about with prevention in between, once we know we’ve gotten rid of what was there. And then if we have to we keep them on longer courses of antibiotics.
Chronic Prostatitis Treatment
Melissa: And what’s the difference between that kind of treatment and how you would approach chronic prostatitis in a male?
Dr. Hlavinka: Again, as my therapy evolved, I saw men for this refractory prostatitis, and I have a big referral practice for this, and I just want to re-emphasize that often chronic prostatitis is an infection that is passed between couples, between members of a couple, because in prostatitis what lives in the semen is representative and that’s the specimen I get.
In the beginning I started out getting urine specimens from the guys and that was helpful but not that helpful. And then I started doing this so-called prostate massage which they hate, but you know, men need some torture just like women every time they go to see doctors, just kidding. But guys are, you know, they’re pretty much weenies and they don’t really put up with that.
The bottom line is, the prostate massage and then having the patient void in a cup afterwards was my next step because that’s what all the books say to do. I know there are particular urologists that think that’s the way to go. I have not found that helpful at all. A semen specimen, if the patient can produce semen, because that comes from the prostate and the seminal vesicle, that’s where the infection lies.
Sample Collection for Prostatitis
So getting that specimen and sending it is absolutely essential as far as I’m concerned, in making that diagnosis. And the same thing with men, is that you’ve got to treat first and see, because most of the time, and this has never been discovered – so I’m getting a brand new organism that’s never been treated – many times with an antibiotic, sometimes a combination of antibiotics for more than one organism and then we see what happens.
Now the prostate has poor antibiotic penetration so it’s difficult to eradicate infection, so it’s important to treat for longer courses than you would, say, for a female UTI. Quite honestly there’s no such thing as a simple UTI in a male. They tend to be almost all complicated when they come to see me. So that’s my practice with that. And my success has been good. I would say people are coming to see me for that reason.
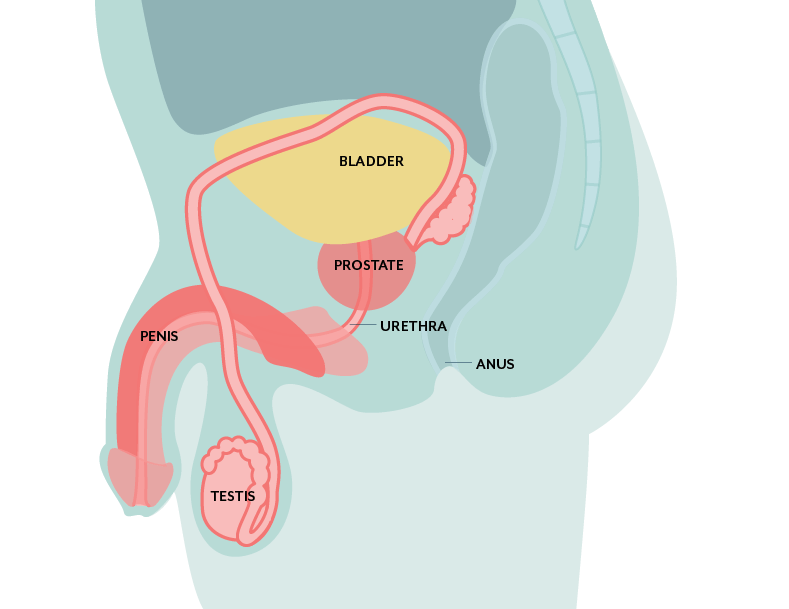
New Treatments for Chronic Prostatitis
Dr. Hlavinka: We even are doing something quite exciting. We’re doing what’s known as intraprostatic injections of antibiotics for those that are very refractory and we’ve had some good success. We now have used a trans-perineal approach, meaning we don’t have to go through the rectum, through the rear end, which really cuts down risk.
This trans-perineal approach with ultrasound guidance and injecting in the prostate is very exciting because I believe a lot of these patients just couldn’t be helped. I have anecdote after anecdote of male patients that just were miserable, couldn’t work, couldn’t function quite honestly. And everybody called them the male version of chronic pelvic pain and no, that wasn’t it. We actually hear from quite a few people in that situation which is why this question has come up and it does seem a difficult thing to treat. Yes it is.
Do People With Recurrent UTI Actually Recover?
Melissa: You said you’ve had some good success with that. Do people with recurrent UTI actually recover? Do you have patients that have recovered from this and are well now?
Dr. Hlavinka: I’ve been doing next generation sequencing three and a half years and I will tell you that the detection is excellent. There is far superior detection of infections at a much more accurate rate than anytime ever before in my career. Am I eradicating infection lifelong because of that new technology? Honestly, Melissa, I don’t know yet.
There are those for whom I need to go back and look at my success rate and document that. That is something I really haven’t done. We’re so thrilled to have this new tool for detection, it’s hard to say ok, let’s not throw out the baby with the bathwater and criticize results when we never had anything like this before. I know it’s better. I know there are people for whom the impact on their health and the quality of life is improved.
They come into my office every day and hug me (before COVID), and I’ve got anecdote after anecdote as I said, of patients for whom this is a life saver, a game changer and a quality of life saver. And for that reason, I would say that yes, there is a chance for a cure. There is a chance for certainly diminishment in impact on quality of life.
How do Implants in the Body Contribute to UTI?
Melissa: We have another question from a couple of members of our audience which is, could a foreign object in the body, such as a breast implant or vaginal mesh, actually be contributing to recurrent UTIs?
Dr. Hlavinka: This is a frequent question and the answer is dependent upon the type of foreign body and where it is, and has there been any incidence of infection before of that implanted material. The issue with say, for instance, an eroded vaginal mesh, that’s unequivocal, yes that could contribute, that’s a simple answer to that one.
The answer to a foreign body such as, say for instance, in an auto accident, and a piece of metal or something like that, and there’s a foreign body that may be impacting the mechanics of an organ, then yes, absolutely, that’s another easy one.
Evidence of an Immune Response to Implants
Dr. Hlavinka: But when you get to things like breast implants, vaginal mesh implants that are functioning well, it’s a little bit more tricky to say that there’s cause and effect. We know that there’s an immune system boost to the foreign implant, even in one’s that have not caused the patient any problems whatsoever – you’ve had it in for years, you don’t even know it’s there – and you remove them and you see this sort of inflammatory rind around them, inflammatory peel around it that the body has walled off.
If you send that to the pathologist, the results are some inflammatory cells, white cells in reaction. I do neuro-simulator implants, and I’ve removed these and I’ve seen that, I’ve seen the tissue as it comes out. So I think that it’s probably a combination of local factors that create a pro-inflammatory response that weakens the immune system.
The breast implant surgeons would tell you that that’s not the case, they feel like they’re sort of the pariahs now in the surgical field. The bottom line is that we’ve had enough patients with these histories of, “I’ve had this condition, it was really bad, or it was worse, got my foreign body removed and my condition is better.”
So to me, that is that sort of anecdotal evidence all of us docs in the era of COVID have learned to pay attention to. To trust our own instincts about a patient and finally listening to people who say my infections are fewer since it was out – there was a reason for that.
Advice on New Treatments for Interstitial Cystitis
Melissa: If people would like to make an appointment to see you are you actually taking on new patients at the moment?
Dr. Hlavinka: Yes I am. Yes I am.
Melissa: And for people who can’t see you, do you have advice for people about how to speak to their own doctor about this problem, and how they can move forward?
Dr. Hlavinka: Perhaps we should include some of the excerpts from this discussion about my experience with the next generation sequencing, my protocols. That’s not to say mine is the right way, I’m very specific in how my practice evolved.
My practice is a fairly unusual urology practice with all these different types of patient populations that have merged to make next generation sequencing quite important to me – essential. But on the other hand I’ve got a lot of experience and would be glad to share it with their providers.
If you’ve found this information helpful, you can support future expert interviews and other projects by contributing to the work that means the most to you. To become more actively involved, become an official Live UTI Free member.
Acknowledgements
Whether or not bacteria and other microbes play a role in Interstitial Cystitis is widely discussed and debated in the IC and UTI communities. More clinicians appear to be adopting the belief that underlying infections play a role in chronic urinary symptoms, while researchers are working to provide answers. We’d like to thank Dr. Tim Hlavinka for generously sharing his time to answer the questions submitted.
More from our expert video series
Watch the rest of our video series with Dr. Tim Hlavinka, or subscribe to Live UTI Free on YouTube.
- UTI And Hormones, HRT And Contraception
- Probiotics And UTI, Biofilms, And The Urinary Microbiome
- How Is Interstitial Cystitis Diagnosed?
- UTI And Sex: Should I Get My Partner Tested?
- UTI And BV, Yeast Infection And Other Risk Factors
To get answers to commonly asked questions about chronic and recurrent UTI, visit our FAQ page. Share your questions in the comments below, or reach out to our team directly.


hello, are there any practitioners in the UK?
Hi Michelle, I have sent you an email. I hope it helps, Molly.
Which probiotics and what are the dosis you recommend to treat IC?
Hi Rocio, we provide information about probiotics for recurrent and chronic UTI, which may be helpful. Melissa
Are there any doctors in the Indianapolis area who utilize similar approaches when treating interstitial cystitis and chronic urinary tract infections? It seems like my urologist cannot do much to help my pain and symptoms. I also feel as though she is not listening to me when I describe what I’ve tried and what doesn’t work. I think it’s time to seek a new provider. Any suggestions?
Hi Natalie, I hope you found the information we emailed helpful. Melissa
Are there any doctors in the New York area who are experienced in using the Urodapter?
Hi Warren, at the moment we don’t have any insights into this. Sorry we can’t be of more help. Melissa