Why Your UTI Test May Be Negative Even When You Have Symptoms
Article by:
Have you had a negative UTI test, even though you have symptoms of a UTI?
Or you might get a positive result, followed by a negative result, even though your UTI symptoms haven’t really improved.
Well, rest assured, you’re not the only one who has experienced this. And even more reassuring, there’s a good chance your test results were wrong, and that you do indeed have a UTI.
Science supports your suspicions that the standard UTI test is inaccurate. It has been proven inaccurate, and this article will help explain why, and what you can do about it.
Jump To Section:
- How accurate are UTI test methods? Not very. >>>>
- Why you can’t trust UTI test strips. >>>>
- 8 Reasons your negative UTI test could be wrong. >>>>
- 5 Alternative UTI test methods you could try. >>>>
- Should You Try Alternatives if you get a negative UTI test? >>>>
How Accurate Are UTI Test Methods?
There are two standard ways to conduct a UTI test:
- A rapid dipstick strip test, which is done on the spot by your medical practitioner (or at home)
- A urine culture, where your sample is sent to a lab and is tested over the course of 24-48 hours.
Despite being the global standards for UTI testing since the 1980s and 1950s respectively, both of these tests are extremely inaccurate. Negative UTI test results can occur, even when individuals have an infection.
Accuracy Of Standard UTI Tests
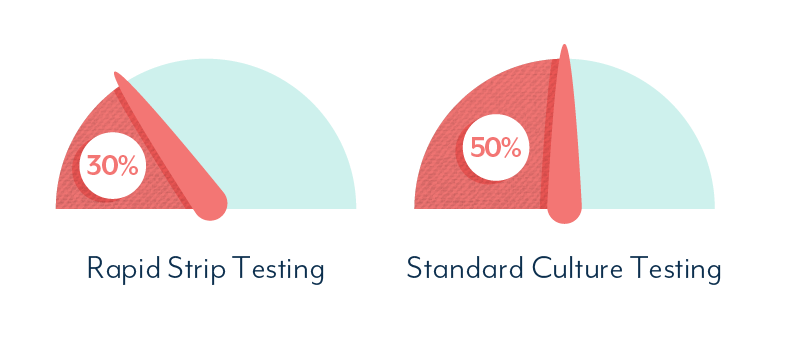
In reality, antibiotics are very often prescribed without any form of UTI test. Patients and doctors are very competent at recognizing the symptoms of a UTI, but there are issues with this approach.
Statistics show that 26-44% of females will experience a recurrence of their first UTI. In this 26-44%, it is likely the initial treatment failed.
Evidence suggests that with each recurrence of UTI, another recurrence becomes more likely.
The more UTIs you have, the more likely you are to get another.
If your UTI treatment failed the first time, it is crucial to find out why as soon as possible, in order to break the cycle of recurrence before it escalates.
Watch our video interview with Dr. Malcolm Starkey to learn more about why standard UTI testing is unreliable.
So why do standard UTI testing methods so often provide negative UTI test results, even when a UTI is present?
First, let’s take a quick look at those urine test strips you can use at home or at the doctor’s office. Then we’ll explain some of the problems with urine culturing done at a lab.
Knowing the issues with both of these tests will arm you with the right questions to ask if you feel like your negative results are wrong.
We’ve also created a free download that provides a breakdown of the different types of testing. Provide the email address at which you’d like to receive the download, at the end of this article. Jump straight to download.
How UTI Test Strips Contribute to the Problem of a Negative UTI Test
UTI test strips are commonly used as an initial indicator for UTI. Studies have shown these test strips are unreliable, and cannot be used to rule out infection.
You’ve probably seen a UTI test strip if you’ve ever been to a doctor for a suspected UTI, but you can also buy them online or over the counter, to use at home.
Home UTI test strips often contain only two of the indicators (the little colored boxes) listed below.

What UTI Strip Test Indicators Mean
| Indicator | Why It’s Used |
|---|---|
| pH Level | If your urine pH is outside the normal range of 5-7, there could be an issue, or your urine pH may have been temporarily altered by something you ate or drank. |
| Protein | Protein in the urine (proteinuria) can indicate kidney disease or other health issues, but it can also be caused by: - Urinary tract infection - Dehydration - Stress or strenuous exercise - Exposure to extreme cold - Fever |
| Sugar | The most common cause of sugar in the urine is diabetes, but it can also indicate other rare health conditions. |
| Ketone | Ketones in the urine can also be caused by diabetes, but can also be a result of a state of ketosis, where the body burns fat instead of sugar for fuel. |
| Bilirubin | Bilirubin in the urine may be an early indicator of liver damage, however, this indicator is known to be highly inaccurate. |
| Urobilinogen | Urobilinogen is a by-product of Bilirubin production and may indicate issues with the liver, among other health issues. |
| Nitrite | Some bacteria that cause UTIs make an enzyme that changes urinary nitrates into nitrites. So if the strip is positive for nitrites, the conclusion is that you have a bacterial UTI. Note that many bacteria do not create nitrites in your urine. |
| Red blood cells (erythrocytes) | Blood can appear in urine due to strenuous exercise, but generally, blood in the urine is taken to be a sign of infection, inflammation, disease, or injury to the urinary tract. |
| White blood cells (leukocytes esterase) | A positive strip result for white blood cells in your urine indicates an infection in your urinary tract, or possibly, kidney disease. |
Studies show that UTI test strips may only be reliable about 30% of the time. This means you may receive a negative UTI test result, and still have an infection.
 | “My urine was visibly cloudy and it burned when I went to pee. My doctor used a UTI test strip in my urine sample and said everything on the test strip was normal. I was told I didn’t have an infection even though I’ve had UTIs before and I know exactly what they feel like.” |
Some studies have bluntly concluded that UTI test strips should be abandoned as a tool for the diagnosis of UTIs in patients with lower urinary tract symptoms.
Given the low accuracy of UTI test strips, if the results are negative but you have UTI symptoms, it would generally be recommended that you have a urine culture test done in a lab.
Which brings us to the next problem…
8 Reasons Your Negative UTI Test Could Be Wrong
Let’s just put it out there that if you have received negative results for a urine culture, but you still have symptoms, it is very possible you have a UTI. Unfortunately, these testing issues can add another layer of confusion and uncertainty when seeking answers.
This happens very frequently, and we can help explain why below. It’s also a good idea to have an understanding of how a standard urine culture works.
Read Ally’s story, ‘An Embedded UTI: More Debilitating Than When it Hurts to Pee’ here.
#1. It Turns Out Urine Is Not Sterile
It has become common knowledge that urine is sterile – it’s even become ingrained in ‘first aid’ advice, like “urinating on a wound is better than using non-sterile water.” But it turns out it’s not.
The bladder has its own unique microbiome, and an ideal balance of microbes that your body does its best to maintain.
Studies have found hundreds of different bacteria in healthy bladders. And in patients with UTIs, they have found even more. That’s a lot of different bacteria that were assumed not to exist in the bladder!
Because UTI test techniques have always assumed urine is sterile, they have always been flawed.
For many, the consequences of this are UTI test results that list ‘contamination’ which implies the bacteria came from a source other than the bladder – possibly skin, vagina, or elsewhere.
This ‘contamination’ may actually be bacteria from inside the bladder that should be considered as part of the puzzle. Results may also show insignificant levels of growth that are then often dismissed.
It’s important to acknowledge here that actual sample contamination is also a real possibility, so minimizing this is also important. We’ve discussed this more below.
#2. The Pathogen/s Causing Your Symptoms May Not Be In Your Sample
Standard UTI test methods focus on free-floating pathogens (which is how UTIs start).
With every recurrence of UTI, there is an increased risk of an embedded, difficult-to-treat bladder infection. An infection embedded in or attached to the bladder wall is called a biofilm.
Biofilms aren’t always bad – many types of bacteria form these structures naturally and they’re an important part of the gut microbiome.
When bacteria form biofilms in the bladder, they are no longer free-floating. If the bacteria are not floating around in the urine, they will not be passed into your sample on urination. Watch our video about bladder biofilms.
If the bacteria are not in your sample, they will not be detected.
There are other reasons your sample may not contain detectable levels of bacteria, including over-hydration. If your bladder is frequently flushed and your urine is diluted, your sample may not contain enough of anything a urine culture can detect.
#3. The UTI Test Was Never Meant To Be Used For Everyday UTIs
In the 1950s a scientist named Kass conducted two small studies on two groups of females with acute kidney infections. One group of participants were pregnant females, the other non-pregnant females.
Kass discovered that a certain concentration of bacteria in a cultured urine sample was enough to indicate a kidney infection with 80% accuracy.
Kass suggested that a kidney infection was present when a certain amount of bacteria was found in the urine. This is called the Kass threshold, and you may have seen reference to it on your UTI test results.
 | The Kass threshold means a concentration of 100,000 (105) colony forming units (CFU) of bacteria per milliliter of cultured urine must be present to indicate an infection. It is a very specific threshold without much room for interpretation. |
The key point here is that the Kass test was already only 80% accurate for acute kidney infections. It was never validated for use in lower urinary tract infections, like bladder or urethral infections.
Yet, this test was embraced by the medical community and has been the global standard UTI test for more than 60 years.
The Kass threshold has since been found to be far too high to detect many lower urinary tract infections. That is, much lower counts of bacteria in the urine can indicate a UTI.
 | “If a urine dipstick or lab test comes back negative but the patient is clearly describing symptoms of a UTI, doctors must listen to them. Urine tests are far from perfect and it is vital to interpret them in the context of the patient’s symptoms.” Dr Jon Rees, Chair, Primary Care Urology Society, UK |
Because modern urine culture tests are based on the Kass test, any bacteria count that is below the Kass threshold will not be considered an infection, and antibiotic susceptibility testing will not be done.
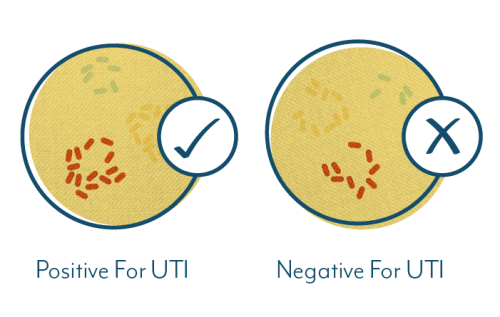
#4. UTIs Can Be Caused By Multiple Pathogens (The Bad Guys)
Another issue with the standard mid-stream urine culture, or Kass test, is that it looks for a single pathogen, and does not take into account the possibility of multiple infection-causing pathogens.
Instead, if multiple pathogens are found, it is generally assumed that the urine sample was contaminated.
This is a problem because some chronic infections have been found to be caused by multiple pathogens co-existing in the bladder. And each pathogen may require a different treatment approach.
 | “Our biological studies reveal mixed microbial infections hiding inside the cells of the bladder. Located there, the microbes seem quiescent but cause low-grade inflammation that may cause various bladder symptoms... Cloistered, inside cells bacteria escape antibiotic and immune attack.” Professor Malone-Lee, Whittington Hospital, UK |
#5. The Standard UTI Test Cannot Grow Most Bacteria
The standard urine culture method does not mimic the environment in the bladder. As we described above, a urine culture uses a specific medium, and specific conditions over a short frame of time.
The vast majority of all known organisms will not grow in these conditions. And many organisms that may be perfectly happy residing and multiplying in the bladder, will not grow in the environment of a culture plate.
This means the standard urine culture methods are just not able to identify all UTI-causing pathogens. And if your UTI is caused by one of these, you will receive negative UTI test results.
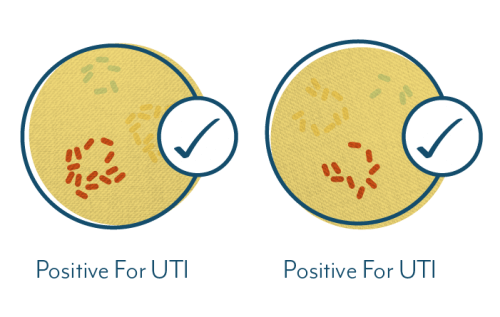
The figure below shows organisms that have been identified in the bladder using expanded culture protocols. The markings can be interpreted as follows:
- Orange stars – Bacteria known to be associated with UTIs or to make UTIs worse, but are not detected by SUC.
- Yellow arrows – Known uropathogens that are not detected by SUC.
- Dark red arrows – Organisms that SUC detects.
- Unmarked – Not much is known about the unmarked organisms. Some of them might be beneficial (like the other Lactobacillus species), some benign (neither good nor bad), and some might be undiscovered uropathogens. More research is needed.

Alternative testing methods, like EQUC, PCR and NGS have been able to identify many pathogens that do not grow in a urine culture.
Dr. Krystal Thomas-White, our scientific advisor here at Live UTI Free, recently offered us additional information about why standard urine cultures can be so inaccurate. She shares these insights and more in our video interview. Check it out!
#6. White Blood Cells In Urine Are Often Ignored
We mentioned white blood cells (leukocytes) in urine earlier, as one of the indicators on a UTI test strip. As much as we cringe at the word, white blood cells are commonly referred to as pus.
White blood cells are also looked for in a standard urine culture at a lab. If either test method detects white blood cells in your urine, it is likely you have a urinary tract infection.
Unfortunately, the presence of white blood cells in a urine culture is measured against a threshold that was established even earlier than the Kass threshold.
You can think of the white blood cell measurement as a backup to the Kass test. Ideally, you would get UTI test results that show a significant amount of bacteria present, PLUS a level of white blood cells that confirms your body is fighting an infection.
Lots of bacteria paired with pus – an immune system response – builds a solid case for a UTI.
There are three major issues with the measurement of white blood cells in a urine sample:
- Much like the Kass threshold, research suggests the threshold for white blood cells is also too high, and that lower levels of white blood cells can indicate a urinary tract infection.
- White blood cells die off quickly outside the body, and may have already significantly reduced by the time a test takes place.
- If your urine contains white blood cells but fails the Kass test, the raised white blood cell count may be considered an anomaly and dismissed as unimportant.
This third point is commonly referred to as ‘sterile pyuria’.
 | Pyuria means pus in the urine, and sterile means the absence of bacteria. So ‘sterile pyuria’ basically means pus was found in the urine, but infection-causing bacteria was not. |
Many researchers believe sterile pyuria is often incorrectly reported due to the Kass threshold being too high, and that lower levels of bacteria may be present and significant.
 | “I had ongoing symptoms. Sometimes acute, sometimes minor, but always there. I bought UTI test strips to monitor my urine. Every single day it showed I had raised white blood cells, but when I sent my urine to a lab, it kept coming back negative for an infection. I had no idea what was going on.” |
#7. Epithelial Cells As An Immune Response Are Overlooked
Epithelial cells are the delicate tissue that can be found lining most of the urinary tract, including the bladder. When you have a UTI, your body can shed epithelial cells as part of its defense against pathogens that form biofilms or intracellular bacterial communities (IBCs).
The body is pretty amazing really. Pathogens invade and start to form communities on and inside the bladder lining cells, and your body starts sacrificing its own cells, in an attempt to foil the plan.
Historically, if these epithelial cells were found in urine that tested negative for bacteria, the cells were considered to be sample contamination. It is now clear that the presence of epithelial cells can actually be an indication of an underlying, embedded infection.
#8. It’s Almost Impossible To Collect An Uncontaminated Urine Sample
If you’ve ever had to provide a urine sample for any type of testing, you’re probably familiar with the terms ‘midstream’ and ‘clean-catch’. These basically refer to a urine sample that is captured only during the middle timeframe of urination and is free from contamination. There are two issues here.
Let’s deal with contamination first. Anatomically speaking, urine exiting the urethra is incredibly likely to pick up bacteria from the surrounding skin and vagina, and this will end up in the sample.
Second, it’s really hard to perch over a toilet, separate the labia (for females), and at the same time have a sample collection cup at the ready, and then only capture 30mL or so of urine from a stream that could be hundreds of milliliters in total.
The result of all this difficulty is that up to 1 in 4 urine samples are considered contaminated. Regardless of the type of testing you choose or are recommended, it’s always best to have an accurate sample.
5 Alternative UTI Test Methods You Could Try
We cannot reiterate enough… No evidence of infection is not the same thing as evidence of no infection.
Or, to put it in a less mind-bending phrase – just because you receive a negative UTI test result, it does not mean you do not have an infection, particularly if the test used was a standard urine culture (SUC).
There ARE other testing options available, ranging from a modified urine culture test, right up to high tech genetic sequencing methods like those described below.
In addition to the information included here, we’ve also covered these testing alternatives in a resource and diagnostic directory you can download and share with your doctor. You can download this resource through our page about how to talk to your doctor about chronic and recurrent UTI or by completing the form below.
Check out our expert video series to learn more about how standard urine cultures are misleading and can lead to an inaccurate diagnosis.
 | “There’s an old expression, if it looks like a duck, walks like a duck, and quacks like a duck. It's gotta be a duck. And so to have somebody who has pain, urgency, frequency and burning, and yet they're told they don't have an infection because a urine culture was negative, who do you believe? Are you treating a lab result? Or are you treating a person?” |
If you’ve received a negative UTI test and feel you’ve exhausted your current options but are still experiencing symptoms that impact your life, it could be time to learn more about how to move forward.
A number of researchers, specialists and doctors in various countries have developed more comprehensive approaches to conditions such as recurrent UTI, chronic cystitis and interstitial cystitis.
Thanks to their efforts, there are a few alternative testing options you may wish to consider.
1. Polymerase Chain Reaction (PCR) Testing For UTI
Polymerase chain reaction (PCR) is one of the more common DNA-based testing methods utilized for UTI. PCR is a very sensitive and specific method used to detect organisms by creating millions of copies of DNA sequences present in a urine sample. The process enables the identification of organisms, but only those selected to be tested for.
The selected organisms form what is called a panel, and for UTI testing this panel can include anything from just a few organisms up to dozens. Because of the limits to how many organisms a panel can contain, there is a risk that the organism or organisms causing a patient’s symptoms will not be included on the panel and therefore not detected.
To help address this possibility, PCR panels for UTI testing typically contain a list of organisms that are most commonly associated with UTI symptoms.
We’ve worked with a few testing laboratories to share more about this testing method and how various labs implement the technology, with UTI patients in mind.
Watch our interview with Dr. Heidi Peterson, who discusses the benefits of PCR testing in her holistic approach to recurrent UTIs, or watch our interview with Dr. Elizabeth Kavaler, who discusses the PCR testing process.
And if you’d like more information to take to your doctor to discuss these tests, you can download our UTI testing resources.
2. Next Generation Sequencing (NGS) For UTIs
Next Generation Sequencing (NGS) is an umbrella term that covers a few different types of DNA-based technologies. NGS testing available for UTI generally utilizes what is called 16s and 18s, which refers to a gene common to all bacteria (16s) and fungi (18s).
NGS is more comprehensive than PCR in that detection is not limited to a panel of organisms. Instead, NGS looks for the 16s and 18s genes among all the genetic material contained within a sample and compares it to a database of thousands of organisms.
Those organisms identified are often reported in terms of ‘load’ which signifies how much of the genetic material found was made up of DNA from a particular organism.
NGS testing is not as widely available as PCR tests, however, it is becoming more accessible as more diagnostic companies adopt this technology.
Digital Microbiology by SBL
In the UK, Digital Microbiology by SBL combines the use of NGS technology alongside minimum inhibitory concentration (MIC) testing to guide antibiotic recommendations. Digital Microbiology offers an at home UTI and vaginal test in which each sample can be collected at home. A clinician’s signature is not required and results are provided directly to you. Learn more about Digital Microbiology.
MicroGenDx
MicroGenDx offers NGS UTI and vaginal tests that ship direct to home and are available in most regions. A clinician’s signature is not required to order a test kit, however, a signature is required to receive antibiotic recommendations. Find out more about MicroGenDx.
BIOTIA-ID Urine
BIOTIA-ID Urine uses shotgun sequencing, which is a comprehensive form of next-generation sequencing (NGS), and artificial intelligence (AI) to detect and analyse organisms in a urine sample. Genetic material in the sample is compared to a database of over 7000 organisms to identify whether any from a list of over 40 uropathogens are present. This test is available in all US states, and Biotia offers a telehealth option for ease of access. Biotia can directly refer patients to clinicians who use their test. Read more about BIOTIA-ID Urine.
A Caveat Regarding DNA-based UTI Testing Methods
Although scientists have used DNA to identify microbes for many years, the technology has historically been expensive and time consuming, and therefore considered inappropriate for everyday testing of chronic illnesses.
This is changing, however, and technologies such as PCR and NGS are now being used to identify the unique DNA of microbes found in human test samples, including urine. DNA-based testing has already detected more than 1,200 different microbial species in urine samples – a number far higher than any other UTI testing method.
Some chronic UTI literate practitioners are wary of DNA-based testing methods, as they often have the ability to detect hundreds of organisms in a single urine sample, and the significance of these organisms is not yet known. Without knowing whether an organism is contributing to UTI symptoms, how can we know which organisms to treat?
To help address this question, DNA-based test results typically show what percent each organism was found in – the idea being that any dominant pathogens will be identified, and that these should be looked at first when it comes to treatment. At this stage, this is the best information we have to go on.
This approach has proven successful for many practitioners who embrace DNA-based testing in different areas of human health, including chronic urinary tract issues.
If conventional methods provide inconclusive or negative UTI test results, DNA-based testing methods such as PCR and NGS could help you find them. It’s always important to find a clinician to work with first.
3. Expanded Quantitative Urine Culture (EQUC)
Expanded Quantitative Urine Culture (EQUC) is a UTI testing method that is relatively new, and has been used in many recent studies around the female urinary microbiome and recurrent UTI.
EQUC uses a modified urine culture protocol, that builds on the standard concept of urine culture with some very important changes. These include using larger volumes of urine, varied atmospheric conditions for incubation and longer incubation times.
The result is that the conditions of EQUC are far superior to those of the standard urine culture.
In fact, one study that compared the two techniques found that EQUC grew bacterial species (was positive) in 80% of the samples tested. In comparison, 92% of these same samples were reported as no growth (negative) using standard urine culture.
EQUC has been adopted as a UTI test method by a selection of practitioners in the USA. We’re looking into where patients can access EQUC and will publish further information as we find it.
4. Fresh Sample Urine Microscopy Test
This test is exactly what it sounds like. Upon providing a urine sample, it is immediately analyzed under a microscope to count things such as bacteria, fungi, white and red blood cells, and bladder lining cells (epithelial cells). It’s a technique that was used in the 1920s and has since been revived.
One UK study focused on recurrent cystitis with negative urinalysis, led by specialist, the late Professor Malone-Lee, used this UTI testing technique in combination with a thorough assessment of symptoms.
Based on positive identification of infection using this technique, the study reported a treatment success rate of 84%, in patients with urinary tract conditions previously considered untreatable.
 | "We do one test; immediate microscopy of a fresh specimen of urine; counting the white and red blood cells, bladder lining cells, bacteria and fungi. The symptoms and the microscopic data are interpreted...they force consideration of all the data particularly the patient's narrative." |
At present, we are unaware of US-based specialists using this same set of testing and assessment techniques. However, it is possible to replicate this technique with the help of a practitioner.
5. Modified Standard Urine Culture Test
While we acknowledge the inaccuracy of standard UTI testing and the frequency of negative UTI test results, some individuals do find an answer. You may be able to request changes to the standard urine culture to increase its accuracy. Possible enhancements include:
- Decrease the colony forming units (CFU) threshold from 105 to 103 or 102.
- Ensure a susceptibility test is completed if your test is positive for bacteria or yeast even at lower levels. This should be done automatically, and is essential to identify which antibiotic or anti-yeast treatment should be prescribed.
- Lengthen the incubation period, to encourage the growth of more types of pathogens.
These changes aren’t always possible, so you should ask your doctor about it, or request it directly at a lab if you test independently.
While we don’t usually recommend using techniques that have been shown to be so flawed, there are very few alternatives in most regions after a negative UTI test, and we don’t want to dismiss it completely.
Why It’s Important To Find The Right Practitioner
While you may be able to request UTI testing independently, the results have limited usefulness without a practitioner who can interpret the information and prescribe an appropriate treatment regimen.
Because the types of UTI testing covered above are not widely available, many practitioners may not be aware of them at all. Or they may be aware of them but have no experience using them, or may believe them to be unhelpful.
Always find a practitioner to work with before ordering testing. We’ve covered recurrent UTI treatment approaches in a separate article, so dive in there for more insight.
 | “With Microbiome testing, you don't often get one bacteria. Certainly, I have found the usual suspects like E. coli. I’ve even detected some STIs, and anaerobes that can’t be grown by culture. Sometimes, you get long lists of bacteria that we know very little about, and I'll do extensive literature searches and sometimes barely come up with one or two papers. And so what I generally do in that situation is to try and figure out which are likely to be pathogenic, and treat those. This is a really different way of prescribing antibiotics compared to when I was trained." |
Should You Try Alternatives If You Get A Negative UTI Test?
Only you can decide how important it is to pursue more effective testing and treatment.
Ask yourself a few questions first:
- Have you already submitted multiple urine samples for culturing in a lab?
- If so, were the results negative despite your symptoms? Did you actually receive your results?
- If your results were positive, do you feel the treatment was effective, or did you experience UTI symptoms again shortly after?
- Do you feel your recurrent or chronic symptoms are something you are happy to manage, or are you interested in investigating a possible long term solution?
- Have you gathered all your previous test results and gone through them with one practitioner to discuss any patterns or trends?
- Do you feel you understand the options available, or should you do some more research?
- Do you have a practitioner that you feel can help with alternative testing methods?
These are all questions we can’t answer for you. We understand this is an individual journey for each person.
To get answers to commonly asked questions about chronic and recurrent UTI, visit our FAQ page.

I’ve had UTI for over two years take medicine and when it’s gone the UTI comes back. Each time they take sample send off and call in another medicine. She looked inside of bladder saw some irritation. Now sending me to Infectious disease Doctor.
Author
Hi Betty, we hear a lot of similar stories. It seems standard urine culturing has failed many people. If you want to chat about it further, you can reach me directly via our contact form. Good luck with the new practitioner! Melissa
Ive never had a UTI but I went in for a routine pregnancy test to be approved for birth control. My doctor came back and asked if i had symptoms because I appeared to have a UTI. When I said no she left it at that. It’s been 2 weeks and I have symptoms (burning, lower abdominal/back pain, frequency), I’ve taken two at home tests that came back positive. I went to get tested to have it treated and the test came back negative at the doctors. I was asked why I was making up symptoms for drugs. I am not understanding why 1) it was positive before and negative now 2) why I have symptoms now and not before but the test results are opposite 3) why a UTI treatment is considered drug seeking?
Author
Hi Nikki, yours isn’t the only story like that we’ve heard – we’ve even heard of people submitting 2 tests in one day, to have one come back negative and another positive. As you’ve read, standard urine culturing can be very inaccurate. Most chronic UTI practitioners do not rely on urine culturing, but will take symptoms into account and use different methods to identify what is causing them. It’s frustrating that your practitioner dismissed your concerns and went as far as suggesting you were seeking unnecessary treatment. Unfortunately, this is also not an uncommon scenario. It can take perseverance to find a practitioner who is willing to investigate deeper. Feel free to reach out via our contact form for more info. Melissa
I tested positive for E faecalis by a NGS test even though a routine urine culture I did the same day came back negative. My E faecalis bladder infection continues even after I’ve taken several antibiotics that the NGS test said it’s been tested/proven to be susceptible to. How could this be? The pain is debilitating.
Author
Hi Kim, sorry to hear your treatment hasn’t been successful yet. Can you send some more information via our contact form so I can share any resources that may be helpful? Melissa
I have been getting a lot of uti’s. About 5 in the past 9 months. I was going to urgent care when I got one. They would give me a prescription for antibiotics and it would go away. Then I would get another one. I recently went to my gynecologist. I told him about my reoccurring uti’s. He told me that was way to many. He sent my urine off for testing. It came back negative for infection. He told me I could have kidney stones or bladder cancer. I’m going in 2 days for an ultrasound on my kidneys. I’m 55 years old. I’m very upset and worried. I just don’t understand why the pain stops and I feel better after I start the antibiotics if it’s not a Uti. What are your thoughts on this. Please let me know. Thank you, Gia Knight
Author
Hi Gia, many studies have shown that the standard UTI culture is inaccurate, and we have heard numerous stories from people who have had negative results, then later found out there was a pathogenic cause for their symptoms. It is possible to receive negative urine culture results while still suffering from an infection. Like you mentioned though, UTI symptoms can have many causes, and it’s very important to work with a health practitioner. If you’d like to chat more about this, you can reach me directly via our contact form. Melissa
Could you please tell me if there are any studies on biofilm “disrupters” like InterFase Plus? Do they work?
Author
Hi Eileen, this is something we’re currently looking into. It seems most studies into biofilm disrupters test action against biofilms in vitro, however, we are unaware of any conclusive studies that support their use against biofilms in the bladder. This is a frequently asked question, so we’ll cover it in as much detail as we can in a future article. If you come across any relevant research in the meantime, please send it our way! Melissa
Hello, I started using Uqora after speaking to my doctor. It helped for about two months. But now I have to call my doctor. It’s back! I have seen two doctors and they really just give me meds and send me on my way. I go to the bathroom before and after sex, I’ve been with my husband for 13 years. I try to drink 100 oz. Of water a day. And really nothing is help. I honestly am starting to give up. If you have any ideas or just anything I can do differently.
Thank you.
Author
Hi Cindy, many people say the turning point was finding the right practitioner. If you’re interested in pursuing this, you can send us a direct message with some information on where you’re based. We may have helpful information we can share. Melissa
It’s so refreshing and reassuring to actually be able to read the facts for once.
I’m 20 y/o and have struggled with UTIs starting at the age of 15, in the last 5 years I have dealt with frustration, shame and accusations of lying about my pain by doctors because of negative results leaving me with self doubt and wondering what is wrong with me and if I’m going to be like this forever. UTIs have been such a recurring problem in my life that I get anxious when I feel one coming on to the point where I will put off a doctor appointment because I’m worried that the results are going to come back negative and my GP will not recognise and listen to my pain.
I wish this information was much more widespread and understood especially by GPs and other health care professionals.
Thankyou for taking the time to put together this article.
Author
Hi Brittany, thanks for the encouraging feedback. I completely understand the anxiety that comes with the constant fear of UTIs. It can take time to find the right practitioner, and I hope you do. You might like to check out the information in our recurrent UTI testing and treatment articles, to see if any of those alternative options resonate with you. We are also working on some resources that may help when you do visit a doctor. If you have any questions or suggestions, feel free to reach out directly via our contact form. We’d love to hear about your progress. Melissa