How is Interstitial Cystitis Diagnosed?
Article by:
How is interstitial cystitis diagnosed? Interstitial cystitis (IC) is an often discussed topic in the recurrent and chronic UTI community. While many aspects of IC are still widely debated, some patients and physicians pursue interstitial cystitis diagnostics and treatment with the guidance of urinary tract infection testing.
Dr. Tim Hlavinka sat down with us to discuss his experience with interstitial cystitis patients and how PCR and NGS testing have been beneficial to his patients.
This video also explains the advantages and limitations of various UTI testing methods.
Watch the video or read the full transcript to learn more.
Jump To Section:
- Video 3 Transcript: Interstitial Cystitis Diagnosis and UTI >>>>
- UTI And Interstitial Cystitis Diagnosis: Standard Culture vs PCR and NGS >>>>
- Understanding When to Treat According to UTI Testing >>>>
- Alive or Dead? DNA Viability Using UTI Testing Methods >>>>
- How Is Interstitial Cystitis Diagnosed? IC Testing Using DNA Technology >>>>
Video 3 Transcript: Interstitial Cystitis Diagnosis and UTI
Melissa: Let’s talk a little bit more about testing. Can you first explain to us why standard urine culture is inadequate, especially for recurrent UTI?
Dr. Hlavinka: Can I, boy can I. I got introduced to next generation sequencing DNA testing three and a half years ago when I was particularly frustrated with a group of my complicated UTI patients and not being able to find answers.
I had the lab throw out a total of seven cultures on a single patient despite the fact that I even called up the head pathologist and asked for special handling of it, to get me an answer. They simply can’t do it. Everything is automated, there’s just no way to change the limitations of traditional (standard urinary) cultures.
A Brief History of Standard Cultures
Let’s go back to high school biology when you first dealt with the petri dish. You had the little petri dish and had a little agar plate on it, which is food for the bacteria, and you coughed in your hand and you took your cotton swab, and you swabbed it on the little agar plate. You waited two days and you watched it grow and said, oh that’s great, look at that!
Look, there’s bacteria growing and there’s different kinds. You have little colonies, little dots grow up. Little white or pink dots grow up. And then they gave you something called penicillin and it looked like a little, tab you put on to stop your bleeding, or, you know, something like that little paper tab. And you put that on there and it’s penicillin, and then two days later you saw the bacteria get killed by it.
That’s how Robert Koch in Germany in 1848 invented cultures. There has literally been no significant change in the technology, other than to automate it, since then. And the automation has made it worse, as I said earlier, because it simply makes it where human beings don’t intervene.
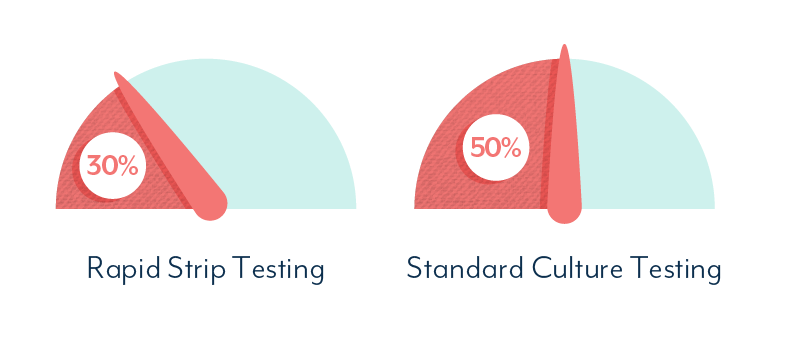
UTI And Interstitial Cystitis Diagnosis: Standard Culture vs PCR and NGS
So the capacity to identify multiple organisms to sub species, to create different time frames for looking at the plates and finding out what’s growing, that just doesn’t exist anymore. And so you’re left with what the lab gives you. You could be charged anywhere from in the United States 48 dollars for a negative culture, to 140 that has multiple organisms that need to be sub-speciated.
When you look at next generation sequencing costs it’s not cheap compared to that but it definitely gives you more information. So that is what the standard urine culture does. And it must be done within two hours, it must be sent within two hours or else.
Melissa: Which must never happen.
Dr. Hlavinka: Right, exactly. You typically have to do a special technique to prep yourself, here you have skin contaminants that make them throw it out. And if you use too much of the little soaps it can kill bacteria so it’s very difficult to get it right. It also has a limitation into the time frame that you can get results back.
Again, now next generation sequencing is getting back pretty quickly such that that’s no longer an issue. And in some places, in the urinary tract infections realm, up to 70% (of cultures) were in error. Maybe even higher numbers were in error, meaning they didn’t find an organism that was there, or they found organisms that weren’t there, that they found, that really weren’t pathogens and were contaminants.
Limitations of UTI Testing Using PCR
Now that is a problem with next generation sequencing too, it is not with PCR, but PCR has the fault of not being able to find something it’s not looking for. Let’s look at polymerase chain reaction or PCR. So PCR is, it’s called polymerase chain reaction and what that’s looking for is amplification of a genetic signal.
You can either use RNA, like they’re doing for the Coronavirus or you can use DNA like we do for most microbes. And you take a little piece of the DNA – a piece of the genetic code – and you have a machine that amplifies it big time and fast, so you can get a read on it.
You’re going to get an identification and you can get an estimation of the number of microorganisms by the amount of genetic material that’s there. So you can identify it and predict how much is there by that, and that’s what PCR can do, But PCR is a probe, meaning it only looks, I should say, it only finds what it looks for.
And if that sounds glib it’s not, because let’s use the analogy of a lego detector right. Let’s say you’ve got a box with, you know, 28000 legos in it. All right. Each of them individual. And you know that your lego is a cube with three prongs, right, that’s two centimeters by two centimeters. So what PCR does is it goes in there and it looks for that exact lego. If it doesn’t find that exact lego, if it’s two by three, it says ‘nothing there guys, nothing to be worried about’, pull out and no lego searching anymore.
Limitations of Next-Generation Sequencing
What next generation sequencing does is it goes in and it says ‘ah oh there’s a peg, okay okay, there’s a side that’s two centimeters, oh there’s another side, there’s a third side okay, it’s a cube. Oh there’s a second peg, there’s a third peg, bingo! E. coli’. And it pulls out the two by two by two three prong lego. And so that is why NGS is so unique and so valuable.
It’s just going to find that that two by two by two three prong lego 99.4 percent of the time accurately, all right. And that’s so important to recognize. Now maybe that particular lego isn’t causing your infection, but at least you know it’s there and that’s what I think is the most important.
And if you’ve got that lego in there, and you know, you’ve got nine million of them, well then you know that you’ve got a problem, all right. And that’s the other thing, so NGS can also give you an estimation of the bacterial load, the microbial load, like PCR can but it’s much more accurate at identifying precisely the organisms that are there.
Understanding When to Treat According to UTI Testing
Melissa: So when it comes to treatment using this kind of technology, is it the bacterial load that really tells you whether something should be treated, or is it the fact that it’s a known pathogen?
Dr. Hlavinka: That is a very, very good question and just, oh my gosh, there are people that, people that want to pay me to give them that answer. So the answer to that is, after doing this for three and a half years with over 800 specimens, the answer is yes.
And I’m not again being glib, but the answer is that a known pathogen in a symptomatic patient with a low bacterial load – I’m going to be cautious and I’m going to treat. And I’m going to do that because if they’re having symptoms, if they’re having symptoms now, you know a little bit of urinary frequency, and it’s a two percent read of E. coli maybe not, but if burning, frequency every 15 minutes, low grade fever, feel terrible, yes I’m going to treat that, because I may have an infection that I failed to treat adequately.
On the other hand, if you have a really high load of something that’s a known contaminant or a known commensal organism – commensal means an organism that normally lives on the body in an unpathogenic way, in a non-infectious way – then I might ignore that, but if they’re symptomatic and that’s the only thing that the NGS gave me, I will treat that too.
And so you can see that – I’ve seen that with Gardnerella in the bladder in women, with Lactobacillus in the bladder, with women where nothing else is there. It’s not a contaminant. There’s a high read, high load and I treat them and they get better.
Alive or Dead? DNA Viability Using UTI Testing Methods
Melissa: That’s interesting. And one question that we get a lot – I’m not sure if you can answer it – but how do you know that the DNA found using this technology is alive, or represented something that was alive?
Dr. Hlavinka: You don’t. You don’t. And again, I deal with symptoms. And the fact is, is that I know that this technology is superior, so the bottom line is that there are there are downsides of NGS and that could be one of them.
But again, in a symptomatic patient when I’ve got the choice between traditional cultures which I know are going to be a fail, and NGS which may give me some false information based on non-viable nucleic acid, I’m going to pick the one that’s going to give me more accurate information.
When UTI Testing Methods are Used in Other Areas of Healthcare
Melissa: So we do see that it’s not exactly standard for clinicians to use this kind of technology for bladder infection, and someone sent in a question that’s very relevant for 2020, which is why are clinicians so willing to use this technology for something like COVID-19, but they are not willing to use it for infection in the bladder?
Dr. Hlavinka: That’s a very good question and if I had the answer, I would have the answer to why clinicians do what they do on a daily basis. I give the example of a stethoscope. Stethoscope is basically the same it’s been for 150 years, just like urine cultures and we haven’t really made that many improvements in it.
What if somebody invented a chip that you put in a stethoscope that made your diagnostic listening to the heart sounds and lung sounds just 98.97% more accurate and you can’t screw it up. You know you’re going to get, and it’ll give you a readout and show you, oh my gosh, you have that S2 sound in the heart, or you’ve got a gallop sound, or you’ve got a murmur and you missed a murmur.
Approach to New UTI Testing Technology
What would happen to stethoscope sales, all right? Old ones would go away, no one would buy them, they would be historically in museums and there’d be a run on stores to get the newest type of stethoscope. So I don’t understand why my colleagues will not incorporate this. It’s not that hard.
It took three months of doing dual cultures and next generation sequencing. When I started this, Melissa, I didn’t know anything about PCR even. So I kind of got PCR and NGS at the same time, which was good for me because then I saw the limitations and benefits of both. But I can certainly tell you that the limitations of traditional (standard urinary) cultures are vast and leaving behind traditional cultures for newer technologies is absolutely essential.
It is not just state-of-the-art, it’s standard of care, and providers that don’t incorporate this into their practice are not practicing state-of-the-art medicine. And I will say that to their face. You can pass this on to them if they need more education about it and its benefits. Send them my email, give them my cell phone. I’ll be glad to talk to them.
How Is Interstitial Cystitis Diagnosed?: IC Testing Using DNA Technology
Melissa: I may do that. We actually receive a lot of emails from people who have been diagnosed with Interstitial Cystitis based on negative urine culture even though they have symptoms that are very similar to UTI. In that case would you say that those people may benefit from pursuing testing with different technology?
Dr. Hlavinka: Absolutely. I’m glad you got into that subject because once again we are looking at a new technology. And maybe that news type of stethoscope tells us about sounds that we never were capable of hearing before, and we have to invent brand new markers and brand new designations and brand new heart sounds and all that because we didn’t know what we didn’t know.
Same thing with next generation sequencing. So we don’t really know what an infection eradication is, to go back to the testing just briefly. Because if I get just a little bit of E. coli and I’ve treated you and have no symptoms, you haven’t had symptoms for a month well I’m not going to chase that. So the negative culture is useless, but do we chase a negative PCR or NGS? I don’t think so. But again, the playing field is changing. These are things that are evolving.
The same thing with the question that you ask is I don’t ever assume that an infection is not a part of the patient’s symptoms until I have a negative NGS. And clearly that doesn’t mean for you know, simple things like passing a kidney stone, which I do in urology. But even then that they can have an infection that’s missed because the stones blocking and we get a little bit of the bacteria beyond the stone.
May Interstitial Cystitis Patients be Dealing with a UTI?

But the bottom line is for things like IC, chronic pelvic pain, chronic prostatitis, pain on intercourse, pain with ejaculation, pain, all these things, I never assume there’s not an infection unless I have a negative NGS. That’s way too many double negatives, but you get the point.
But again, it is changing the playing field for what I see is fully 50% of my IC patients and probably more than 50%. I would say probably the majority, probably 55% of my IC patients have a detectable, significant load organism that I treat and improve symptoms. In many of them it’s allowed me to take them off medication.
It was the problem all along, all right. Now some of them that fail, I scope and then we do the ulcer check and things like that. But the bottom line is that until you do an NGS and whether or not it’s catheterized or voided, that’s a controversy too, but until you do an NGS and it’s negative I don’t call it IC anymore. And I believe those criteria should change soon.
Interstitial Cystitis Improvement after DNA Testing
Melissa: That was going to be the next question: If you have had patients with previously diagnosed IC that have been found to have infection and have subsequently been treated and symptoms have resolved.
Dr. Hlavinka: Yes, the answer is yes.
Melissa: One final question on the testing is, do you think it’s important to test both the vagina and the urinary tract when there’s chronic UTI symptoms?
Dr. Hlavinka: Yes, there’s never a good doctor who won’t take more information. Now what we do with it is different, it may be different, but there’s never a good doctor that won’t take more information. And I love information and this has given me information I never had before.
If you’ve found this information helpful, you can support future expert interviews and other projects by contributing to the work that means the most to you. To become more actively involved, become an official Live UTI Free member.
Acknowledgements
Interstitial cystitis is a familiar topic for our community. How interstitial cystitis is diagnosed depends on the clinician. Many believe that IC is a difficult to detect infection, however, additional research is greatly needed in this area. We’d like to thank Dr. Tim Hlavinka for generously sharing his time to answer the questions submitted.
More from our expert video series
Watch the rest of our video series with Dr. Tim Hlavinka, or subscribe to Live UTI Free on YouTube.
- UTI And Hormones, HRT And Contraception
- Probiotics And UTI, Biofilms, And The Urinary Microbiome
- New Treatments For Interstitial Cystitis, UTI And Prostatitis
- UTI And Sex: Should I Get My Partner Tested?
- UTI And BV, Yeast Infection And Other Risk Factors
Share your questions in the comments below, or reach out to our team directly.

