UTI and Menopause: Estrogen May Improve Recurrent UTI
Article by:
For many people, UTI and menopause go hand-in-hand. But why is post-menopausal UTI a thing? Can estrogen help for recurrent UTI? And is estrogen cream safe?
We get a lot of questions about hormones, hormone therapy and the possible connection to recurrent UTIs.
Many people who reach out to us have noted they experience UTI symptoms at certain times of their menstrual cycle or that the frequency of UTIs increased at the onset of menopause. Others found starting or stopping the contraceptive pill had an impact.
So is there a link between hormones and recurrent UTI, and can we do anything about it?
Jump To Section:
- UTI and menopause: The vaginal and urinary microbiomes. >>>>
- How a healthy vaginal microbiome impacts recurrent UTI. >>>>
- Recurrent UTI and menopause may be linked by estrogen levels. >>>>
- Estrogen vs. antibiotics for UTIs. >>>>
- How estrogen impacts the bladder. >>>>
Why Did My Doctor Prescribe Hormones For My UTIs?
You might be surprised to find out that if you are post-menopausal and have recurrent UTIs, your doctor might prescribe hormone replacement therapy (HRT).
This could be estrogen in either systemic form (a pill that is taken orally) or topical form (a cream that is applied inside the vagina).
Why would estrogen help when it comes to UTI and Menopause? Let’s start with how the vagina and urinary tract are linked.
UTI And Menopause: The Vaginal And Urinary Microbiomes
The relationship between UTI and menopause has a few layers. First, let’s just confirm something many people are not yet aware of…
Contrary to long-held beliefs, urine is not sterile. The bladder has its own unique microbiome, even in a healthy state.
To be fair, the discovery of the female urinary microbiome was fairly recent, but the consequences of this research are already making ripples through everything we thought we knew about UTIs.
When we mention that the bladder has its own microbiome, most people think of what they have learned about the gut microbiome. This conjures images of a complex network of millions of bacteria all living and working together.
The bladder is very different from the gut; its function is to store and remove waste products.
It is a low biomass niche, meaning instead of billions of bacteria, a healthy person’s bladder may only have a few thousand. And instead of a community of different bacteria, a healthy person tends to have one or two dominant bacteria.
 | “You could think of the gut microbiome kind of like a rainforest, filled to the brim with different species of plants and animals. If the gut is a rainforest, the bladder is a desert. It has a microbiome, but it’s low biomass, meaning there are relatively few bacteria to be found there.” |
UTI And Menopause: The Interconnected Urinary And Vaginal Microbiomes
Based on the knowledge that the bladder and the vagina have their own microbiomes, you may be asking yourself whether the two can influence one another.
It does look like the bladder and vaginal microbiomes are interconnected. The same types of bacteria are found in both anatomical sites (Lactobacillus, Gardnerella, Staphylococcus, Streptococcus, etc).
And the exact same strain of bacteria have been found in both sites of individual females. Therefore it is possible for a population of Lactobacillus to live in both the vagina and bladder at the exact same point in time.
Read about Cindy’s experience of UTI during menopause here.
The Microbial Communities Of The Urinary Tract, Vagina And Gut

This means that at the species level it is possible that these microbiomes are connected, but when we look at the microbial community of each location as a whole, we still find differences.
 | “Talking about finding the same strains of bacteria in both the vagina and the bladder is like saying that we found a species of evergreen tree growing in the lush river valley and high up on the dry mountainside. We all know that there are other plants that will not normally grow in both environments. So does the presence of the evergreen tell us more about the tree, or the environment in which it grows? And can we take those same lessons and apply it to an invasive species?” |
These are the types of questions we’re still trying to answer, with regard to the urinary microbiome.
How Organisms Move From Your Gut To Your Urethra
As you may know, the main theory about how recurrent UTIs occur, goes something like this…
Organisms that exist within the digestive tract can end up very close to the opening of the vagina, thanks to our bowel movements and wiping habits.
Given the proximity, it can be very easy for these organisms to attempt to colonize the vagina.
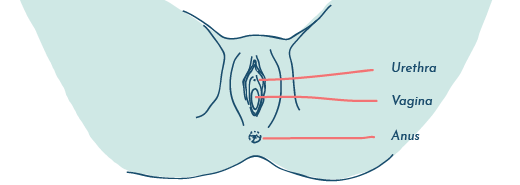
If they successfully colonize the vagina, they’re then in a good position to do the same in the urinary tract.
It may be the case for some people, that an imbalance in the vaginal microbiome causes a continuous flow-on effect to the urinary tract, resulting in frequent UTIs.
How A Healthy Vaginal Microbiome Impacts Recurrent UTI
There are a few different types of bacteria that live in the vaginal tract. The most common are Lactobacillus species such as Lactobacillus crispatus, Lactobacillus gasseri, Lactobacillus jensenii, Lactobacillus iners, however other Lactobacillus species can routinely be detected.
Other organisms are also commonly found, and include Gardnerella vaginalis, Corynebacterium, Aerococcus, Atopobium, Streptococcus, Staphylococcus, Peptostreptococcus, Prevotella, Pseudomonas, Megasphaera, Sneathia, and many others .
Which Bacteria Are Good And Which Are Bad?
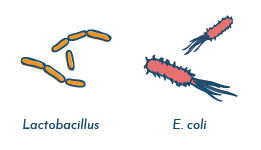
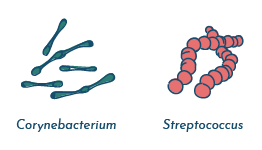
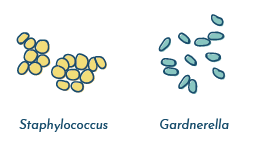
There is debate in the scientific community whether any of these bacteria can be considered pathogenic (disease-causing) in the vaginal tract.
This is a fairly new field, but is seems that healthy women with different ethnic backgrounds tend to have different vaginal bacteria, suggesting that there is a wide range of microbiome profiles for healthy women. Meaning that there isn’t one single bacteria or bacterial community that is right for everyone.
However, the prevailing medical dogma still considers the most beneficial of these bacteria to be Lactobacillus – those listed above.
These bacteria grow to high numbers and produce lactic acid and hydrogen peroxide as a byproduct. These byproducts make it really hard for uropathogens, such as E. coli, to grow in the vagina.
This means, when Lactobacillus is present in high enough numbers, E. coli cannot ascend from the gut into the vagina. If E. coli can’t get that far, then it therefore isn’t anywhere near the urethra, and is less likely to reach the bladder.
You can learn more about the current state of your vaginal microbiome with a vaginal swab test that looks at the entire microbiome. Companies like Evvy provide a detailed report about the microbiome community type and what this could mean for healing.
Recurrent UTI And Menopause May Be Linked By Estrogen Levels
So where does estrogen come in? How are UTI and menopause linked?
It is thought that estrogen increases the stores of glycogen on the surface of the vaginal epithelial cells (vaginal lining).
Glycogen acts as a food source for Lactobacilli. The more glycogen that is available, the more the Lactobacilli eat, and the more they multiply. And as mentioned above, abundant Lactobacilli provide a lactic acid rich, protective environment.
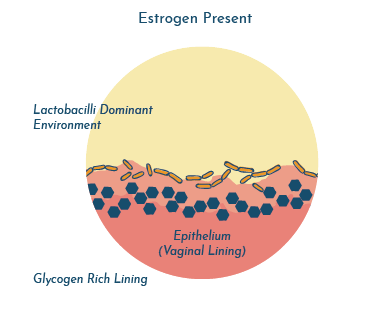
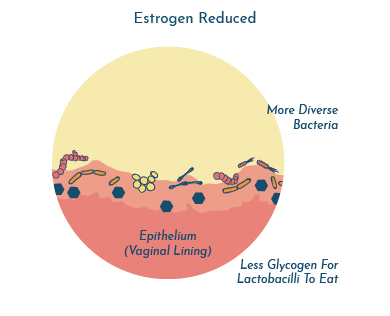
When females go through menopause and the levels of estrogen are reduced, this food source also diminishes, and so do the Lactobacilli and accompanying protective acid.
UTI And Menopause May Be Directly Linked To Lactobacillus In The Vaginal Microbiome
What happens after menopause? Studies have shown that post-menopausal females tend to lose Lactobacillus and their vaginal microbiomes become more diverse2-4.
This change can be influenced by Hormone Replacement Therapy (HRT).
Studies have shown that post-menopausal females who have been on HRT for years tend to have more of a Lactobacillus dominant community compared to females of the same age not on HRT.
Estrogen vs. Antibiotics For UTIs
In the late 90s and early 2000s, a series of studies was done around UTI and menopause. They compared estrogen therapy (applied vaginally) to prophylactic antibiotics (preventative antibiotics every day).
The studies looked at which therapy was more effective at preventing recurrent UTIs after menopause.
One study in particular looked at the use of topical estrogen cream vs. prophylactic antibiotics in post-menopausal females.
This study found that without any treatment, the participants experienced an average of 5.9 UTI episodes per year. With estrogen treatment, that dropped to 0.5 episodes per year compared to 0.8 episodes per year with an antibiotic.
How Estrogen Impacts The Bladder
Despite the research that has already been completed around UTI and menopause, there is a lot that is still not understood about the link between estrogen and the urinary tract. And therefore the link between UTI and menopause.
First of all, we don’t know the effect that estrogen has on the bladder microbiome.
It’s one thing to demonstrate that estrogen in post-menopausal females may reduce the recurrence of UTI. It’s another thing entirely to completely understand why this happens, and the long-term impact of its use.
We do know that estrogen can improve the bladder epithelium (the lining of the bladder). But studies are still ongoing to see if estrogen has a similar effect on the bladder microbiome as we see with the vaginal microbiome.
Secondly, we don’t entirely understand how the Lactobacillus is getting access to the glycogen in the vaginal tract. So it is possible that estrogen is doing something other than simply providing a food source.
Thirdly, for women who go from a high diversity vaginal microbiome without estrogen to a Lactobacillus dominant microbiome on HRT, we don’t know where the Lactobacillus is coming from. How is it getting re-populated?
Finally, we don’t know why some women who have perfectly good estrogen levels still get UTIs.
Watch our interview with Dr. Philippe Zimmern, who discusses what the urinary microbiome look like post-menopause, and the role of estrogen therapy in the urinary microbiome.
Is Estrogen Cream Safe?
As with all medications, the first thing you need to do is check with your doctor. Based on your medical history and risk factors, estrogen therapy may not be the best choice for you.
However, for the majority of people, a topically applied cream or pessary is perfectly safe. These forms of medication keep the hormones to a localized area, so carry fewer risks than a pill (which circulates the hormones throughout your body).
Watch our interview with Dr. Rachel Rubin on vaginal estrogen therapy to learn more about safety, efficacy and long term benefits:
What The Estrogen UTI Link Means For Recurrent UTI Sufferers
For those who experience recurrent UTI post-menopause, it may be worth raising the topic of estrogen therapy with your doctor.
We’ve linked the references for this article above, so you can review any relevant studies and share them with your doctor if you’d like to.
For pre-menopausal sufferers of recurrent UTI, the link between the vaginal and urinary microbiomes is still likely to be important.
For this reason, we’ve covered current research into the use of vaginal probiotics for recurrent UTI, and we’re working on some content specifically about this topic.
It’s also significant that a link between hormones and recurrent UTI has been established. We look forward to further research that will help enlighten us on how this link may impact pre-menopausal sufferers of recurrent UTI.
Learn more about UTI and hormones in our expert video series.
If you have questions or comments about UTI and menopause, you’re welcome to share them below. To get answers to other commonly asked questions about chronic and recurrent UTI, visit our FAQ page.

This article makes perfect sense to me. I have been supplementing with probiotics on a daily basis for many years now but it’s been a couple of months since I started getting flatulence so I included kombucha and enzymes in my diet thinking that i might have dysbiosis due to antibiotics that I’d taken for cystitis. I had been using Estradiol 25mcg 3 times a week for a couple of years then the doctor reduced it to 10mcg 3x a week and I noticed discomfort during intercourse. I had no idea that this could be related to more bouts of cystitis.
Hi Xenia, we hear from a lot people with similar experiences that have found estrogen cream helpful. It’s clear that we need more research into this area! Melissa
WOW. I have no history of UTIs and suddenly got one that I cannot get rid of. The bacteria that continuously coming back is enterococcus faecalis and it will not eradicate!!! I’ve been on 5 different rounds of antibiotics all of which it was supposed be sensitive to but it remains and my symptoms persist. Strangely, this happened two months after I got off my birth control pill that I had been on for years! Any advice for me? My husband and I were wanting to start a family but now… I feel I have to wait until I get healthy but the likelihood feels like it is slipping away…
Hi Lizzy, can you send us a direct message with this information and let us know where you’re based? Melissa
Great info here. What is the opinion on Utiva? Thank you.
Hi Sarah, we don’t provide information about specific products, though we do have some info about cranberry for UTI, which I believe Utiva is based on. Melissa
I used estrogen suppositories to soften the tissues of my Urethra, but found it to difficult to keep up with, so my doctor prescribed eString which is inserted and left inside the urethra. Could not decide whether that was helping much, but it had a bad effect on my mammograms, so I was told to remove the eString. I haven’t gone back to it, and want nothing more to do with estrogen.
Hi Emily, thanks for sharing your experience. More research is definitely needed into recurrent UTI treatment approaches and who they may or may not be suitable for. Melissa
Great article. Thank you! Could this apply to women with PCOS also?
Hi Antonia, that’s an excellent question. I haven’t seen any studies specifically linking this, so I’ve added it to our list of questions to ask an expert. Given the hormonal link to recurrent UTI, it seems plausible. Melissa
What is the role of testosterone treatment
( small daily dose of cream) in relation to UTI for post menopausal & naturethroid women /patients?!!
Hi Cathy, we don’t yet have any information regarding testosterone treatment for UTI. If you have any useful resources we can start looking into, can you send us a direct message? Thanks, Melissa
Can having the Marina(I think that’s how you spell it !) coil fitted for menapausal problems be a cause of a U T I ?
Hi June, we haven’t seen any research into this, but we have received similar questions from others who are speculating whether it may be linked to symptoms they are experiencing. If you have any other questions, you can always get in touch directly. Melissa
As always very informative and in a format that is understood,thank you
Hi Maria, thanks for your positive feedback! Melissa
Can you tell me the differences with compounded estriol cream and the regular estrogen creams like estrace? I’m being treated for e faecalis and citrobacter in urine with antibiotics. Suffered with painful bladder syndrome for 7 years. Also given compounded estriol( I’ve had breast cancer) the estriol is weaker, I’ve been told so may take 3 months to work. My oncologist also told me about a new product Imvexxy which has a lower estrogen content than estrace and premarin. Obviously considering my history I want the lowest estrogen possible but still need it to work. Any thoughts? Thanks
Hi Lesley, that’s a great question and I’ve added it to our list for the experts. We share their answers periodically via our mailing list. If you’d like to join the list, you can do so above, at the bottom of the article. If you have any other questions, feel free to send them to us directly. Melissa